High cholesterol can contribute to fatigue, but not in the way most people expect. It doesn’t spike your energy one day and drain it the next.
Instead, elevated LDL and triglycerides quietly restrict circulation, trigger low-grade inflammation, and strain the heart over months or years.
The number that matters isn’t dramatic. The tiredness it causes usually isn’t either, which is exactly why it gets missed.
| Disclaimer: This article is for informational and educational purposes only. It does not constitute medical advice. Always consult a qualified healthcare provider before starting a new exercise, nutrition, or wellness program, or if you have concerns about your cholesterol levels. |
The Real Connection Between High Cholesterol and Fatigue
When LDL rises above 130 mg/dL and begins depositing into artery walls, the body responds with inflammation.
That inflammation is metabolically expensive. Your immune system is running in the background, spending resources on a problem you can’t feel yet.
On top of that, plaque-narrowed arteries reduce the volume of oxygen-rich blood reaching muscles and the brain. Less oxygen in means less usable energy out. It’s a straightforward equation, even if the timeline is slow.
A 2020 study published in the journal Multiple Sclerosis and Related Disorders found that a higher total cholesterol-to-HDL ratio was significantly associated with increased fatigue severity scores.
Separately, research on patients with chronic fatigue syndrome found elevated lipid peroxidation markers alongside lower HDL levels, suggesting that lipid imbalances directly affect cellular energy production.
These aren’t marginal findings. The link between an unfavorable lipid profile and persistent low energy is real, even if it isn’t linear.
What this means practically: if your LDL is elevated and you’re consistently tired without an obvious cause, cholesterol is a legitimate variable to investigate, not dismiss.
Types of Cholesterol and How Each Affects Your Energy
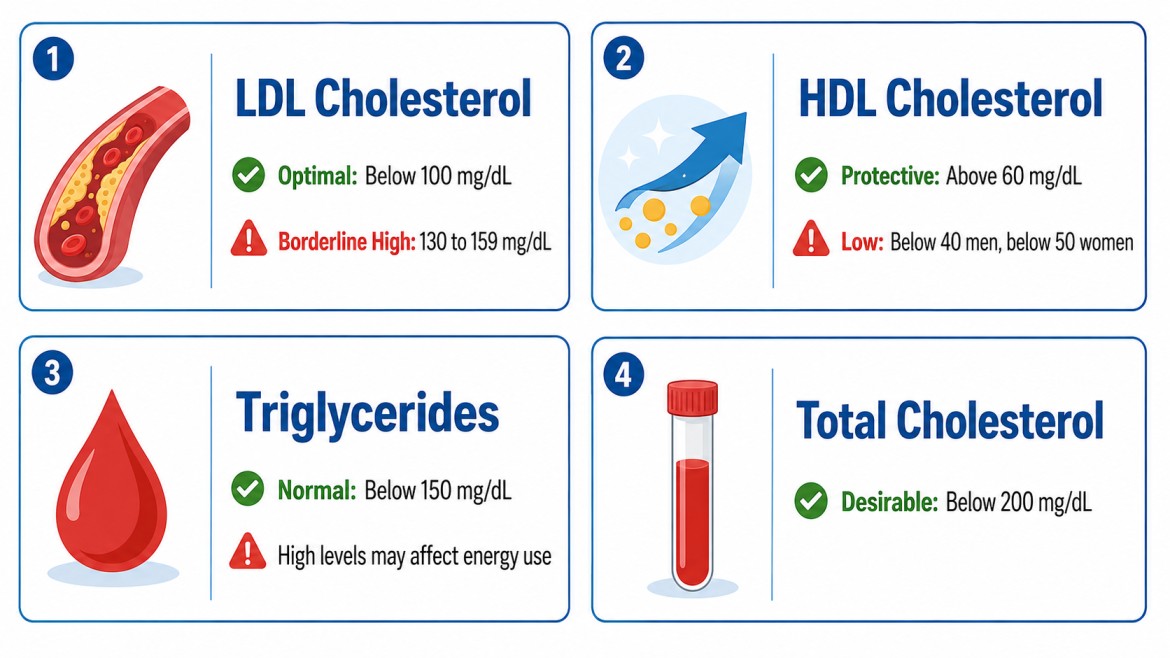
Not every cholesterol number causes fatigue the same way. Understanding which marker is doing what helps you and your doctor make smarter decisions.
LDL Cholesterol: The Primary Driver of Arterial Damage
When LDL exceeds 130 mg/dL, the surplus begins to deposit into arterial walls and initiates the formation of plaque.
Over time, this narrows the arteries, forces the heart to work harder against greater resistance, and progressively reduces oxygen delivery to working muscles and organs.
The result is a cardiovascular system operating at reduced efficiency, and that inefficiency shows up as fatigue.
Optimal LDL is below 100 mg/dL according to the American Heart Association.
Above 160 mg/dL, the risk of arterial damage and associated symptoms, including persistent tiredness, rises substantially.
HDL Cholesterol: The Clearance Mechanism
HDL does the opposite of LDL. It removes excess cholesterol from the bloodstream and arterial walls and returns it to the liver for removal. Higher HDL is protective.
The threshold that matters: below 40 mg/dL in men and below 50 mg/dL in women is considered low and is associated with increased cardiovascular risk.
Research among multiple sclerosis patients found that higher HDL was directly associated with lower fatigue severity scores.
Think of HDL as the clearance rate for the buildup that causes fatigue. A low clearance rate means the problem compounds faster.
Triglycerides: The Overlooked Energy Disruptor
Triglycerides are not technically cholesterol, but they appear on every lipid panel and matter for fatigue.
Elevated triglycerides, typically above 150 mg/dL, thicken the blood and impair the body’s ability to use fat efficiently for fuel.
They also correlate strongly with insulin resistance, which compounds fatigue by disrupting how cells convert glucose into usable energy.
Foods highest in saturated fat and refined carbohydrates are the main dietary drivers of triglyceride elevation.
Cutting processed sugar and white flour often produces a faster drop in triglycerides than cutting dietary fat does.
Why High Cholesterol Causes Fatigue: The Mechanisms
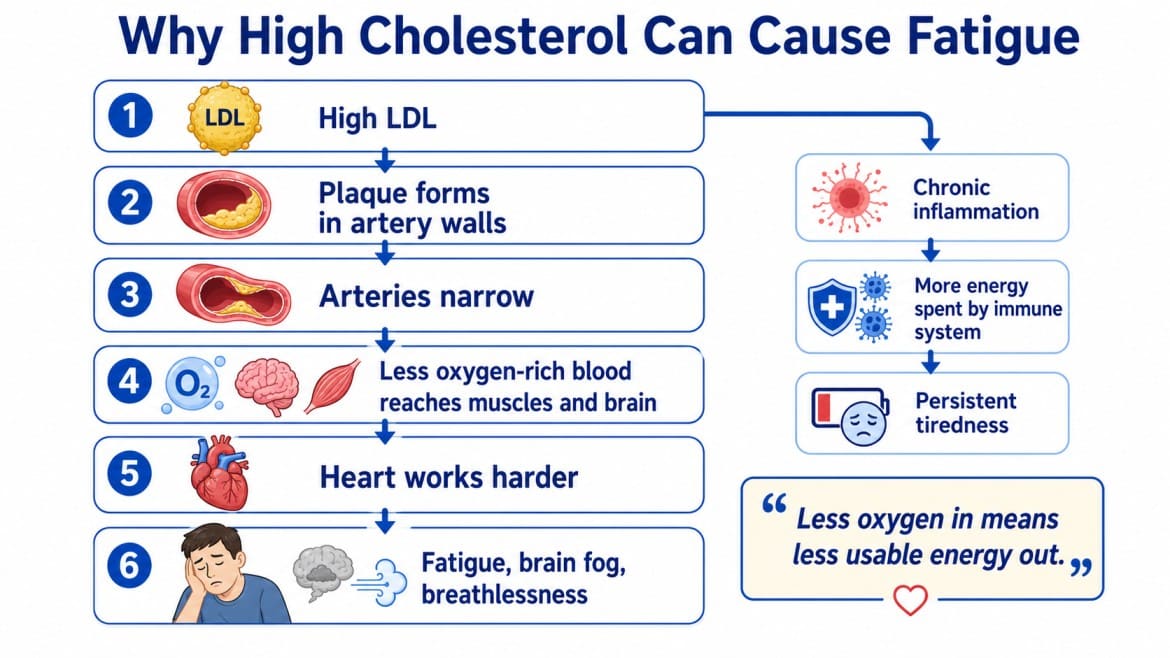
Several processes run in parallel once cholesterol levels become elevated. Understanding each one explains why the fatigue can feel so diffuse and resistant to rest.
Chronic Inflammation
Excess LDL in arterial walls triggers an immune response that doesn’t resolve. The body dispatches white blood cells to the affected arteries, and that immune activity runs continuously.
Chronic inflammation is one of the most energy-intensive states the body can sustain. It elevates cytokine production, disrupts sleep architecture, and keeps the nervous system in a low-level alarm state that drains reserves without any noticeable cause.
A 2017 consensus statement from the European Atherosclerosis Society confirmed that LDL is a direct driver of this inflammatory cascade.
Reduced Oxygen Delivery
Plaque-narrowed arteries carry less blood per heartbeat. Less blood means less oxygen delivered to skeletal muscle and the brain.
Muscles under even moderate exertion, such as climbing stairs or carrying groceries, hit their oxygen ceiling faster than they should.
The brain, which accounts for roughly 20% of total oxygen consumption despite being only 2% of body weight, is particularly sensitive to circulatory inefficiency.
Brain fog, difficulty concentrating, and slow mental processing are all downstream symptoms of reduced cerebral oxygen delivery.
Heart Strain
A narrowed arterial network means the heart must generate higher pressure to move blood through it. This sustained overexertion is similar, physiologically, to running with a partial airway obstruction.
The heart can compensate for a long time, but at a metabolic cost. That cost is felt as systemic fatigue, particularly during and after physical activity, and eventually at rest if the strain continues unchecked.
Mitochondrial Damage from Oxidative Stress
Elevated cholesterol increases free radical production in the bloodstream, and those free radicals cause oxidative damage to cell membranes and mitochondria.
The mitochondria are where ATP, the body’s primary energy currency, is manufactured. Research on chronic fatigue syndrome patients found elevated malondialdehyde, a marker of lipid peroxidation, alongside lower HDL levels.
Damage to mitochondrial membranes directly reduces the body’s capacity to generate and sustain energy at the cellular level.
Sleep Disruption
High cholesterol is associated with an elevated risk of obstructive sleep apnea, a condition in which airway obstruction leads to repeated microarousals throughout the night.
These arousals fragment slow-wave and REM sleep, the stages most critical for physical recovery and cognitive consolidation.
Poor sleep then compounds the fatigue already being generated during the day by the mechanisms above, creating a cycle that worsens over time.
Symptoms of High Cholesterol-Related Fatigue

High cholesterol fatigue has a specific character that distinguishes it from ordinary tiredness. If several of the following patterns sound familiar, getting a lipid panel is a logical next step.
Fatigue That Does Not Resolve with Sleep
Ordinary tiredness improves with a full night’s rest. Fatigue driven by poor circulation does not improve with rest because the underlying problem is not a sleep deficit.
It’s an oxygen and nutrient delivery deficit. You wake after 7-8 hours and still feel heavy, unmotivated, and slow to get going.
This pattern, sometimes called non-restorative sleep when sleep apnea is involved, is one of the more consistent reports from people whose fatigue turns out to have a cardiovascular component.
Exertional Symptoms: Breathlessness and Muscle Fatigue
When plaque narrows the arteries, the supply of oxygenated blood to working muscles becomes limited.
Activities that previously felt easy, such as a brisk walk, carrying bags up a flight of stairs, and cycling a familiar route, begin to feel disproportionately demanding.
The muscles reach fatigue threshold more quickly because they receive less fuel.
The heart compensates by beating faster, which can produce a noticeable or uncomfortable awareness of effort that was not there before. This is one of the earlier physical signals that arterial circulation has been compromised.
Cognitive Slowness and Brain Fog
The brain depends on consistent, high-volume blood flow to maintain sharp function.
When circulation is impaired, the first symptoms are often subtle: slower processing, difficulty finding words, reduced ability to sustain concentration, and a sense that thinking requires more effort than it used to.
These symptoms are easily attributed to stress or aging, which is why they often go uninvestigated for years. In the context of elevated LDL or low HDL, they warrant specific flagging.
Physical Signs of Cholesterol Buildup
In some cases, high cholesterol produces visible signs. Xanthelasma, small yellowish deposits that appear near the inner corners of the eyes or on the eyelids, indicate cholesterol deposits beneath the skin and are associated with elevated LDL.
Xanthomas, similar deposits that form over tendons or joints, particularly the Achilles tendon and knuckles, are a marker of severe hypercholesterolemia.
Leg pain or cramping during walking, known as intermittent claudication, is a symptom of peripheral artery disease caused by cholesterol-narrowed leg arteries.
These physical signs, when present, make cholesterol the obvious investigation, but they appear in only a minority of cases. Most people with high cholesterol have no visible signs at all.
Does Fatigue From High Cholesterol Become Permanent?
If high cholesterol remains untreated long enough to cause structural arterial damage, some loss of circulatory efficiency can persist even after cholesterol levels are brought under control.
Atherosclerosis involves changes to the arterial wall itself, not just what’s circulating in the blood. That said, the cardiovascular system retains significant capacity for improvement when cholesterol is managed early.
Studies on statin therapy have documented reductions in inflammatory markers and patient-reported energy levels alongside LDL lowering, particularly when intervention occurs before significant plaque burden has accumulated.
Early detection and consistent management give the body the best chance to maintain healthy circulation and energy levels. Waiting until symptoms are severe before testing significantly limits what’s reversible.
Statins and Fatigue: A Complication Worth Knowing
This is a section most cholesterol-and-fatigue articles skip, and it matters. Statins are the most commonly prescribed treatment for high LDL, and fatigue is a documented side effect in a subset of users.
The mechanism involves two pathways: first, the same process that lowers cholesterol production also reduces the body’s synthesis of CoQ10, a coenzyme central to mitochondrial energy production.
Second, statins can cause muscle pain or myalgia, which disrupts sleep and leaves some people feeling chronically sore and drained.
If you start statin therapy and your fatigue worsens rather than improves, that is not a sign the medication is working. It is a side effect worth discussing with your prescribing doctor.
Common solutions include adjusting the dose, switching to a different statin formulation, timing the dose at night rather than morning, or discussing CoQ10 supplementation.
Statin-related fatigue is manageable for people who experience it. It should not be assumed to be permanent or unavoidable.
| Note on Statins: If you are currently on statin therapy and experiencing new or worsening fatigue, report it to your doctor before making any changes to your medication. Stopping statins abruptly can cause a rebound increase in LDL. The fix is almost always a dosage or formulation adjustment, not discontinuation. |
How to Lower High Cholesterol and Restore Energy
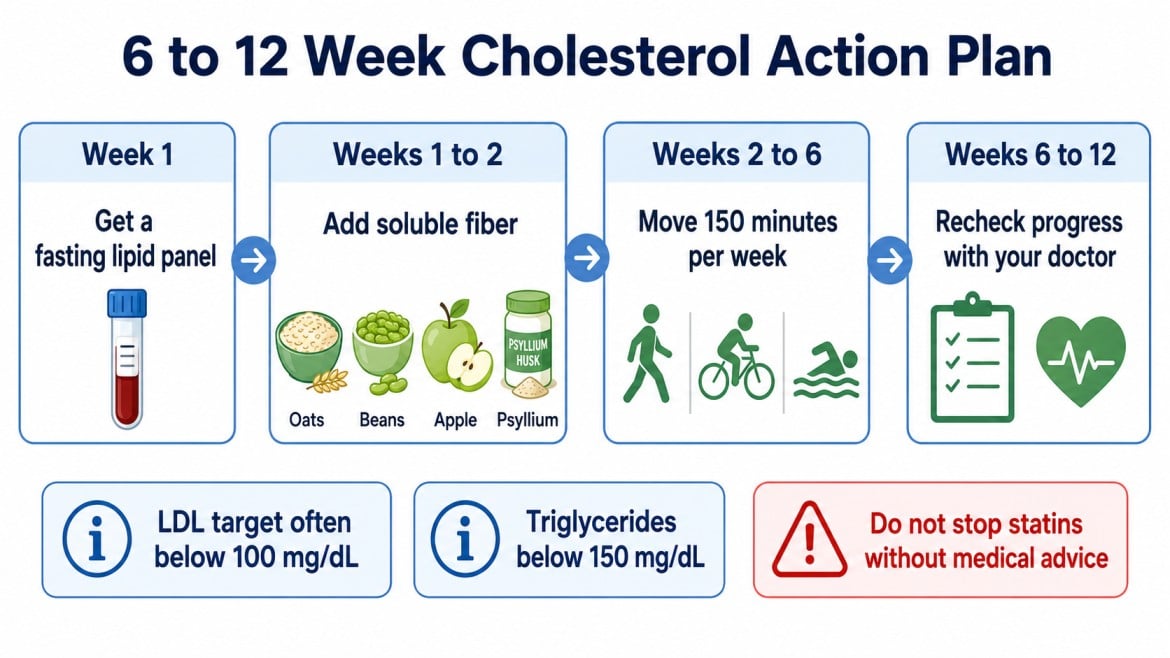
Managing cholesterol is one of the most well-studied interventions in preventive medicine, and the dietary levers are specific enough to produce measurable results within 6-12 weeks of consistent application.
Dietary Changes with the Strongest Evidence
The dietary moves that consistently lower LDL and triglycerides are: increasing soluble fiber (5-10 grams per day from oats, legumes, apples, and psyllium), replacing saturated fat with unsaturated fats like olive oil and nuts, and cutting processed sugar and refined carbohydrates to lower triglycerides.
A structured calorie-conscious meal plan that prioritizes whole foods, lean protein, and fiber is one of the fastest practical ways to apply these changes.
Adding omega-3 fatty acids from fatty fish (two 3-ounce servings per week) or fish oil specifically lowers triglycerides and supports HDL.
Foods like salmon, sardines, and tuna, which are rich in the omega-3 fatty acids that support cardiovascular health, are among the highest-value additions here.
Plant sterols, found in fortified foods or supplements, block cholesterol absorption in the gut and can lower LDL by 7-10% when consumed consistently at around 2 grams per day.
Exercise: The Fastest Way to Raise HDL
Aerobic exercise is the single most effective lifestyle tool for raising HDL. In my reading of the research, the evidence is clearest for moderate-intensity activity sustained over time rather than high-intensity bursts.
The American College of Sports Medicine recommends 150 minutes per week of moderate-intensity aerobic activity, which is enough to produce meaningful HDL increases within 8-12 weeks.
Walking, cycling, and swimming all qualify. Resistance training provides additional benefit by improving metabolic health and insulin sensitivity, which in turn lowers triglycerides.
Medications and Supplements
Statins remain the first-line pharmacological option for elevated LDL and have the strongest evidence base for cardiovascular risk reduction.
When statins are not tolerated, ezetimibe and PCSK9 inhibitors are alternatives. Omega-3 supplements at prescription doses (4 grams per day) are FDA-approved for reducing severely elevated triglycerides.
Berberine and red yeast rice have some evidence of modest LDL-lowering effects, but should be used under medical supervision given their statin-like mechanisms and potential side effects. None of these supplements replaces medication in high-risk individuals.
Monitoring: Know Your Numbers
A fasting lipid panel gives you four numbers: total cholesterol, LDL, HDL, and triglycerides. The number that matters most for cardiovascular risk assessment is LDL.
Target below 100 mg/dL if you’re at risk; below 70 mg/dL if you have confirmed heart disease. HDL above 60 mg/dL is considered protective. Triglycerides below 150 mg/dL is normal range.
The American Heart Association recommends testing every 4-6 years for adults without risk factors and annually for those with elevated risk or existing cardiovascular conditions.
High Cholesterol Fatigue vs Other Causes: A Simple Diagnostic Frame
Fatigue has many causes, and not all persistent tiredness points to cholesterol. Here is a practical way to think about it before your next doctor’s visit.
Cholesterol-related fatigue tends to begradual in onset rather than sudden, worsens with physical exertion, is accompanied by shortness of breath or leg heaviness, and is present alongside risk factors like age over 45, family history, or a diet high in saturated fat and refined carbohydrates. It does not respond to extra sleep. It may be accompanied by brain fog or reduced exercise tolerance that was not there a year ago.
Fatigue more likely from other causes is sudden onset, tied to a specific life change or stressor, accompanied by mood symptoms (more likely depression or anxiety), responsive to better sleep hygiene, or present with other specific symptoms like unexplained weight change or cold intolerance (more likely thyroid).
The overlap is real, and cholesterol doesn’t exclude other causes. But if your fatigue fits the first pattern and you haven’t had a lipid panel in the last two years, getting one is the most efficient next step you can take.
Frequently Asked Questions
Does High Cholesterol Make You Tired?
Yes, indirectly. High cholesterol doesn’t cause fatigue through a single acute mechanism, but elevated LDL and triglycerides trigger arterial plaque buildup, chronic inflammation, and reduced oxygen delivery to muscles and the brain, all of which produce persistent tiredness over time. The fatigue is typically gradual and doesn’t resolve with rest because it stems from circulatory impairment rather than a sleep deficit.
Can High Cholesterol Cause Fatigue and Weakness?
Yes, both can occur together. Reduced blood flow from plaque-narrowed arteries limits the oxygen and nutrients reaching skeletal muscle. Under even moderate exertion, muscles hit their fatigue threshold faster than normal. Physical weakness, particularly during activities that were previously easy, is one of the earliest signs that arterial circulation has been compromised by elevated cholesterol. Leg heaviness or cramping during walking (intermittent claudication) can also occur when the arteries supplying the legs are affected.
What are the Symptoms of High Cholesterol in Women?
High cholesterol is largely asymptomatic until arterial damage has accumulated. When symptoms do appear, they are similar in women and men: persistent fatigue unresponsive to sleep, shortness of breath during moderate activity, reduced exercise tolerance, brain fog, and occasionally visible cholesterol deposits (xanthelasma near the eyes). Women tend to have higher HDL levels than men before menopause, but HDL drops significantly after menopause, increasing cardiovascular risk substantially. Any of these symptoms in a post-menopausal woman with no recent lipid testing warrants a fasting cholesterol panel.
Does High Cholesterol Cause Brain Fog?
It can. The brain consumes roughly 20% of the body’s oxygen supply and is highly sensitive to circulatory efficiency. When plaque narrows the arteries supplying the brain, reduced blood flow impairs concentration, slows processing speed, and makes sustained focus difficult. Chronic inflammation, another consequence of elevated LDL, also affects brain function by elevating cytokines that disrupt cognitive performance. Brain fog is not a classic or reliable symptom of high cholesterol, but in the context of cardiovascular risk factors and no other explanation, it’s worth investigating.
Do Statins Cause Fatigue?
In some patients, yes. Statins reduce the body’s production of CoQ10, a coenzyme involved in mitochondrial energy production, which can cause fatigue and muscle discomfort in a subset of users. If statin-related fatigue is a concern, solutions include timing the dose at night, adjusting the dose or switching to a different formulation, or discussing CoQ10 supplementation with your doctor. Do not stop taking statins without medical guidance, as cholesterol levels can rebound quickly.
How Quickly Can Fatigue Improve After Lowering Cholesterol?
Patients on statin therapy who report energy improvements typically notice them within 6-12 weeks of treatment, alongside a measurable drop in LDL and inflammatory markers. Dietary changes that reduce LDL by 10-15% generally take the same amount of time to show metabolic effects. Significant reversal of arterial plaque takes longer, but even partial reductions in inflammation and improved circulatory efficiency can produce noticeable energy improvements before structural changes occur. The earlier treatment begins, the more the body can recover.
What is a Normal Cholesterol Level?
According to the American Heart Association, a desirable total cholesterol is below 200 mg/dL. LDL below 100 mg/dL is optimal; 100-129 mg/dL is near optimal; 130-159 mg/dL is borderline high; 160 mg/dL and above is high. HDL below 40 mg/dL (men) or 50 mg/dL (women) is low and increases risk. Triglycerides below 150 mg/dL are normal. These targets may be adjusted downward by your doctor if you have additional cardiovascular risk factors or existing heart disease.
Summary
The numbers on your lipid panel can directly affect how you feel every day, and that connection is missed far more often than it should.
High cholesterol doesn’t make you tired overnight, but elevated LDL quietly narrows arteries, drives chronic inflammation, and reduces the oxygen your muscles and brain depend on.
The fatigue that results is real, gradual, and worth taking seriously. If your energy has declined without explanation and you haven’t had a fasting lipid panel recently, that test is the most efficient place to start.
A total cholesterol above 200 mg/dL or an LDL above 130 mg/dL, paired with persistent fatigue, warrants intervention, whether through dietary changes, exercise, medication, or a combination of all three.
Sources
- American Heart Association, “Cholesterol.” https://www.heart.org/en/health-topics/cholesterol
- Correale M et al., “HDL cholesterol and fatigue in multiple sclerosis patients.” Multiple Sclerosis and Related Disorders. 2020. PubMed.
- European Atherosclerosis Society Consensus Panel, “Low-density lipoproteins cause atherosclerotic cardiovascular disease.” European Heart Journal. 2017. doi:10.1093/eurheartj/ehx144
- American College of Sports Medicine, “Physical Activity Guidelines.” https://www.acsm.org








